Improved MRI for Carbon Monoxide Diagnosis
The value of MRI for carbon monoxide diagnosis is increasing each year. Improved MRI resolution provides the images with greater detail[1]. Shorter scanning times makes the images sharper. New MRI protocols are providing better information about brain function. While these improvements have only improved the imaging findings for other brain damage, it has changed the landscape for the use of the MRI for Carbon Monoxide cases.
For Our Treatment of Brain Damage after CO click here.
MRI and other diagnostic tools are not stand alone tools for to diagnose brain damage after carbon monoxide. The exception is that lesions in certain areas of the brain are so specific for carbon monoxide that it may be the only thing on the differential diagnosis.[2] In understanding the role of MRI for carbon monoxide poisoning, it is important to understand that CO poisoning starts as an ischemic event, where the initial damage is from hypoxia. Hypoxia and its more severe cousin anoxia are caused by failure of a cell to get enough oxygen. Carbon monoxide takes the place of oxygen in the blood and thus brain cells can be asphyxiated. As the blood is circulated through the body evenly, one might expect to see symmetrical damage on MRI. But that is a misunderstanding of all of the causes of brain damage from carbon monoxide.
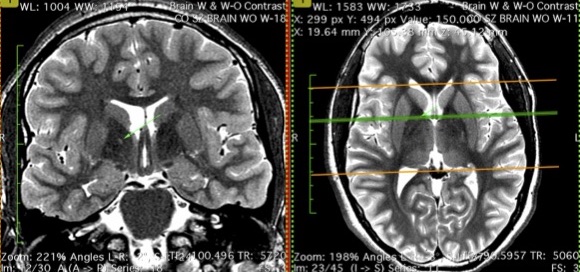
This image shows different views of the same globus pallidus lesion after carbon monoxide poisoning. This is a unilateral globus pallidus lesion.
But the bilateral nature of hypoxia is only a small part of the brain damage that occurs after CO poisoning. It is believed that inflammatory mechanisms and immunological over-response – which goes on for days or weeks after the poisoning – causes the most brain damage. The body senses CO as a poison and over reacts to this poison in destructive ways. As MRI technology has evolved, far more lesions are found and those lesions are just as likely to be one sided as bilateral.[3]
Understanding the Alphabet Soup of Diagnosis
Modern diagnostic tools involve more than the MRI but the alphabet soup of these diagnostic tools can get quite confusing. They include the following traditional tools:
- CT – Computerized Tomography. CT is an extremely valuable tool for brain injury diagnosis but less valuable for CO poisoning. CT is the first imaging study that will be ordered in almost all cases of trauma, including carbon monoxide poisoning.CT’s limitation is that it primarily identifies intracranial pressure events and large scale bleeds. It will miss most smaller hemorrhages and lesions. For more on the use of CT after brain injury, click here: http://subtlebraininjury.com/ct-after-concussion/
- MRI – Magnetic Resonance Imaging. See below for detail on MRI.
- EEg – a decades old tool that will identify electrical abnormalities in the brain. It is not nearly sensitive enough to identify all brain damage. See http://subtlebraininjury.com/eeg-after-concussion/
- PET Scan – Positron Emission Tomography. PET is a decades old functional test, with limited availability because it requires nuclear isotopes. It also has far worse resolution than MRI. PET scans are not nearly as sensitive as MRI at identifying the type of brain damage after a carbon monoxide event. SPECT scans have even worse resolution. For more: http://subtlebraininjury.com/pet-scan-after-concussion/
- Electronystagmography. ENG is a valuable diagnostic tool for diagnosing dizziness, balance and vertigo pathologies. These tools evaluate the function of the vestibular system and typically administered by ENT doctors, such as otolaryngologists or neuro-otologists. Vestibular function tests can be an integral part of diagnosing the pattern of neurological deficits found in CO cases. For more http://vestibulardisorder.com/eng.php
- VEP – Visual evoked potentials. This is a test of the optic nerve transmission and can be a key finding after brain damage, particularly CO caused brain damage. This test can identify reduced visual processing speed and is often a clear indicator of brain damage.
MRI for Carbon Monoxide – Newer MRI Protocols
Each generation of imaging the quality of the scans gets better. With each improvement in MRI, resolution improves, new protocols are developed, more brain damage from carbon monoxide poisoning is identified. As an MRI is a digital machine, the generations can be short on some improvements and much longer on others. New protocols are developed often. It takes a much as 10 years for the magnets themselves to be updated, as MRI scanners are expensive machines. The smallest lesion a 3Tesla MRI can see is approximately 1 mm. Thousands of axons can be damaged in an area that small and still not show up on even the best scanner used for clinical use today.
The state of the art MRI includes the following sequences:
- T1 and T2. On T1 images, the cerebral spinal fluid (“CSF”) is black. On T2 images, the CSF is white. (T1 and T2 are not to be confused with 3T – which is short for 3-Tesla, which is a measurement of the strength of the magnet.)
- T2 Flair – This is a T2 image where the CSF is black, but and is superior at seeing certain types of pathologies, including White Matter Hyperintensities. (Yes that gets confusing.) For more: http://mriquestions.com/t2-flair.html
- Axial, Coronal and Sagital views, preferably of each of the above sequences. Axial images are taken as is looking down at the head, top to bottom. Coronal images are shot as if looking straight at the face, from front to back. Sagital images are is looking at the brain from the side, from one ear to another.
- DWI –Diffusion Weighted Imaging. DWI is a sensitive test for CO in the first day or two after the poisoning. Its value as a diagnostic tool for CO is reduced because rarely is it ordered on the day of the poisoning. DWI is valuable for diagnosing ischemic strokes, because it is one of the first things that is ordered acutely. DWI lacks any sensitivity more than 4 days after the ischemic event.
- DTI – Diffusion Tensor Imaging. DTI is a used to identify damage to fiber tracts in the brain. Fiber tracts are collections of axons running together throughout the white matter of the brain. DTI has been around for more than 15 years and should be included in all brain damage studies.
- SWI and other Hemosidrin studies. SWI stands for susceptibility weighted imaging. Hemosidrin are the iron deposits that are left behind after a brain bleed. Hemosidrin are not new but the SWI is far more sensitive than the gradient echo protocols that preceded it.
- Brain Volume studies, such as NeuroQuant. These studies measure and image in color the 3 dimensional volume of all brain structures.
- MRS – Magnetic Resonance Spectroscopy. This is a protocol that measures the metabolites usage within the brain.
- fMRI – Functional MRI. fMRI can see in real time, the type of brain dysfunction historically only seen on PET and SPECT scans. fMRI offers far superior resolution to PET and is a real time test, where the technician or neuroradiologist can actually watch the brain think and process.
- Perfusion studies. These studies are functional tests that can identify blood perfusion into different areas of the brain.
Brain Atrophy On MRI
Though neurons are too microscopic to be imaged by even advanced MRI magnets, when countless neurons and axons die in a structure, that structure becomes smaller. When a structure shrinks, the CSF will occupy more area around that structure. Thus, brain atrophy can be seen on an MRI. NeuroQuant can show these losses statistically. In addition, neuroradiologists can diagnose brain volume loss independently.
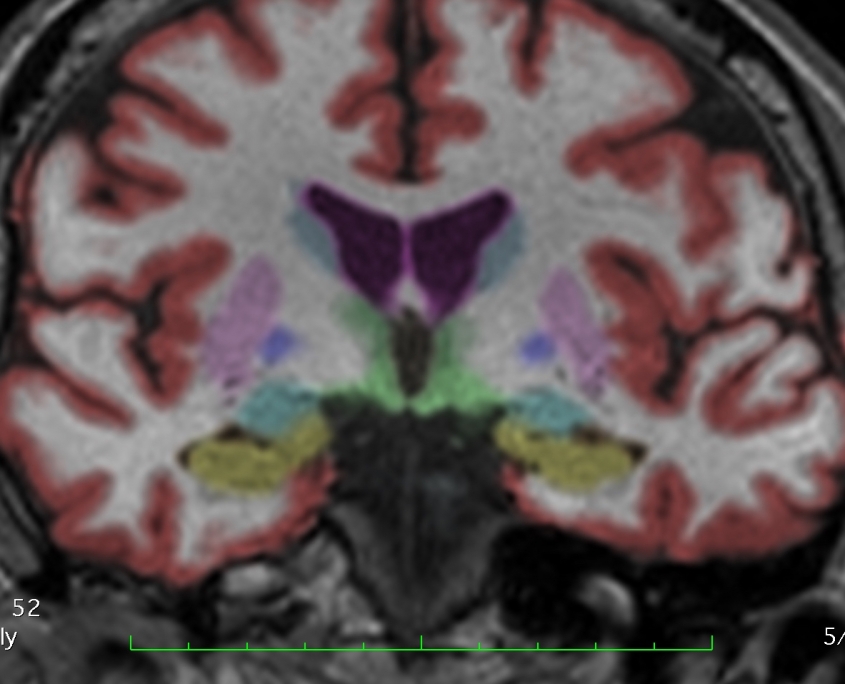
The sensitivity of MRI for carbon monoxide diagnosis is rapidly increasing as new protocols are developed. Shown here is a coronal NeuroQuant image.
An area that volume loss is identifiable is the hippocampus, which is normally surrounded by temporal horns, which CSF filled areas. When the hippocampi get smaller, the temporal horns get bigger. Temporal horn enlargement their enlargement is easy to spot, especially on coronal sequences. A neuroradiologist should always look for temporal horn enlargement.
[1] A decade ago, most clinical scanners were still 1.5 T scanners, meaning 1.5 Tesla, a unit of measurement for the strength of the magnet. Today most clinical scanners are 3T.
[2] Basal ganglia lesions are the highly specific finding for carbon monoxide poisoning.
[3] Basal ganglia lesions following carbon monoxide poisoning HOPKINS, el. al. Brain Injury, March 2006; 20(3): 273–281.
