Carbon Monoxide is a Poison – Not Just an Oxygen Deprivation Event
800-992-9447
Carbon monoxide is a poison, but too the medical community doesn’t grasp that there is a poisoning component involved, different than asphyxiation of cells from oxygen. Most deaths from carbon monoxide occur because of asphyxiation of the heart muscle from oxygen. Carbon monoxide binds to hemoglobin and 27 times the rate that oxygen does, meaning that carbon monoxide takes the place of oxygen in the blood. When carbon monoxide takes the place of enough oxygen, the bodies organ that has the most immediate need for oxygen, will stop beating, that being the heart. Death almost always follows if immediate treatment is not received.
But the overwhelming majority of people do not die from carbon monoxide exposure. Those who do not die, except in the most extreme cases (such as in someone who suffered a heart attack) will largely recover from the lack of oxygen to the cells, the hypoxia event. Since the body recovers so quickly from the lack of oxygen in survivors, medical personnel too often discharge carbon monoxide survivors as soon as the blood levels return to normal. A typical discharge note will say something like:
Upon admission to the floor, headache resolved. Continued complaint of light headedness. The decision was made to continue oxygen. A repeat carboxyhemoglobin was 1%. As she was then asymptomatic, she was discharged.
What this ignores is the poison part because carbon monoxide is a poison. This person did suffer DNS. This person did have an abnormal brain MRI, proving that brain damage occurred, after this person was discharged from the initial hospitalization.
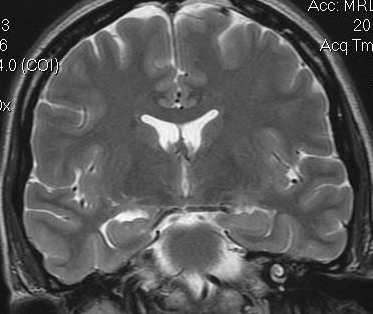
The above MRI shows the effect of carbon monoxide as a poison, as hippocampal atrophy is shown. The wishbone white shape on the bottom left side of this image shows an increase in size of the temporal horn, which happens when the hippocampus shrinks, due to brain damage after carbon monoxide poison.
The body has an entire defense mechanism designed around protecting it from poisons. Unfortunately, that defense system in too many cases can overreact and cause more damage than the quantity of the poison would account for. A bee or wasp sting does not carry enough poison to kill a human being. Yet people die from such stings. The reason they do as the sting causes anaphylaxis, a severe allergic reaction. We understand anaphylaxis because it happens so commonly and have developed effective treatment, particularly the use of epinephrine, which has been mass produced in a ready to use pens.
The nature of the immune response to carbon monoxide does not cause the shut down of the heart in the same way as anaphylaxis, and while it can damage any cell in the human body, it primarily causes brain damage. But because the effects of escalating brain damage are much more subtle than heart stoppage, there has been little recognition that an emergency which can cause irreparable harm in continuing. If untreated, this brain damage can continue to worsen for days, even months.
Carbon Monoxide is a Poison that Causes DNS
Traditionally there has been a term for such condition: delayed neurological sequelae or DNS. See, Guiseppe Peppe, Delayed neuropsychological sequelae after carbon monoxide poisoning: predictive risk factors in the Emergency Department. A retrospective study. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3065430/ According to this article,
DNS usually develops within weeks after an initial clinical recovery from acute poisoning. The reported incidence varies widely from 3 to 40%, because of the lack of established diagnostic criteria.
Most frequently described sequelae include a broad spectrum of neurological deficits, cognitive impairments and affective disorders. DNS gradually resolve over the the first months but can be permanent …Patient’s initial presentation does not predict the development of delayed neurological sequelae with certainty, but some variables have been associated to DNS.
Other studies have found the incidence of DNS to happen in more than 40% of the cases, with how high the COHb level is above 10% not being a relevant finding.
Is there an EpiPen® for DNS? Probably. Hyperbaric oxygen therapy, if administered on the day of exposure can be quite beneficial. While the medical community has avoided a bright line standard requiring hyperbaric oxygen therapy, we believe this is antiquated thinking. Countless times, people with quite severe COHb levels, as high as 50, have had satisfactory recoveries. In contrast, 40% or more of those with COHb levels as low as 10 have had permanent deficits from DNS. The real incidence of DNS is likely unknown because the criteria for finding DNS is in dispute. A review of the dispute over hyperbaric oxygen therapy will be discussed in other blogs.
What are the symptoms of DNS?
According to Peppe article, the Presenting symptoms of DNS are notoriously aspecific. They can include headache, asthenia, vomiting, nausea, transient loss of consciousness, altered mental status. “Correct diagnosis is a challenge for the emergency physician.” In essence, if any of the types of symptoms that might have warned an individual that they were subject to carbon monoxide poisoning at the time of the incident reoccur, they are likely feeling the effects of DNS. What we do know is that DNS causes significant brain damage. In the process of fighting off the perceived threat of that carbon monoxide is a poison, the bodies immune system keeps attacking cells. Brain cells are among the most vulnerable and are also the least likely to regenerate. While alternative work arounds may exist for such brain damage, such work arounds often leave permanent neuropsychological deficits, because the work arounds are far less efficient than the original neural pathways.
In future blogs we will discuss a more detailed description of what can occur in the delayed onset of brain damage from carbon monoxide poisoning.

i need help so desperately my poor sister and mother was exposed and is still in coma like state please tell me what can i do
Please call my office at 800-992-9447.
Attorney Gordon Johnson